hygiene-precision: distributor of Aquolab products
Bleeding gums: What are the causes and how to treat them?
Bleeding gums is a common problem that can have various causes, ranging from simple irritation to more serious conditions. Here is some important information about it.
hygiene-precision.com
3/2/202614 min read
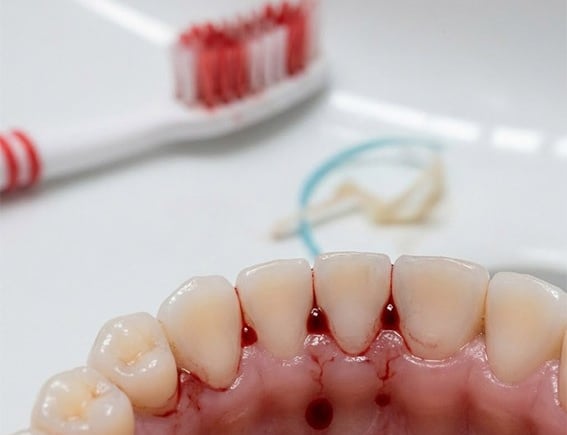
🔹 Bleeding gums for no apparent reason: gingivitis ?
Gingivitis is an inflammation of the gums that is most often caused by a buildup of dental plaque a sticky film of bacteria that forms on the teeth and along the gumline. If plaque isn’t removed through proper brushing and cleaning, it can irritate the gums and lead to gingivitis.
Gingivitis: symptoms
Bleeding gums, especially when brushing or using dental floss.
Red, swollen, tender gums.
Bad breath or an unpleasant taste in the mouth.
Gum pain or discomfort.
Sometimes the gums may recede, making teeth more sensitive.
Bleeding gums causes: gingivitis
Dental plaque buildup: The main cause of gingivitis is the accumulation of plaque, a sticky bacterial film on the teeth. If it isn’t removed regularly through correct brushing and cleaning, it can trigger gum inflammation.
Insufficient brushing: If teeth aren’t brushed properly, food debris and plaque remain and irritate the gums.
Poor oral hygiene: Lack of consistent oral care (brushing and interdental cleaning) allows plaque to harden into tartar (calculus), which worsens gingivitis.
Smoking: Smoking weakens immune defenses and makes gums more vulnerable to infections, including gingivitis.
Medications: Some medications can affect gum health, especially those that reduce saliva or those used for specific conditions (for example, anticonvulsants).
Hormonal changes: Hormonal fluctuations (pregnancy, menopause, menstruation) can increase gum sensitivity and the risk of gingivitis.
Chronic diseases: Diabetes and other health conditions can also raise the risk of gingivitis.
Bleeding gums: natural approach for gingivitis
Improve oral hygiene: Brush twice daily with a sonic soft-bristled toothbrush and a fluoride or ozonated toothpaste. Prefer an ozone water flosser for optimal oral hygiene. If you use floss to remove plaque between teeth, be careful not to cut into the gums. Water flossers with controlled pressure are gentler on gum tissue.
Dental visit: A professional cleaning removes plaque and tartar that a toothbrush can’t eliminate.
Antibacterial mouthwash: An antiseptic mouthwash can help reduce plaque and the bacteria responsible for inflammation. Be cautious with mouthwashes that are too harsh on oral tissues.
Diet changes: A balanced diet rich in fruits and vegetables can support the immune system and help maintain healthy gums.
Bleeding gums: preventing gingivitis
Brush at least twice a day and use an ozone water flosser daily.
See a dentist for a professional cleaning at least once a year.
Avoid smoking and maintain a balanced diet.
If you notice gingivitis symptoms, consult a dentist promptly to prevent the inflammation from worsening.
To summarize, gingivitis is usually reversible when caught early and treated properly.
However, if left untreated, it can progress to periodontitis a more serious form of gum disease that can lead to tooth loss.
🔹 More significant gum bleeding: periodontitis ?
Periodontitis is a more advanced form of gum disease that typically develops from untreated gingivitis. Unlike gingivitis, which affects only the gums, periodontitis also damages the supporting structures of the teeth, including the periodontal ligaments and the alveolar bone that keep teeth in place. If left untreated, periodontitis can lead to tooth loss.
Periodontitis: symptoms
Bleeding gums: Gums often bleed when brushing or using floss.
Swollen, red gums: The gums may become more swollen, red, and tender.
Persistent bad breath: Chronic halitosis can be a sign of periodontitis.
Gum recession: Gums pull back, exposing tooth roots and increasing sensitivity.
Loose teeth: Teeth may become mobile or shift because supporting tissues are damaged.
Pus between teeth and gums: Abscesses can form, causing pain and pus.
Teeth “getting longer”: Progressive loss of support can make teeth appear to loosen or become exposed.
Bleeding gums causes: periodontitis, a more advanced stage
Plaque and tartar: As with gingivitis, periodontitis is mainly driven by plaque buildup. If plaque isn’t removed, it hardens into tartar and can intensify gum inflammation. When inflammation becomes severe, it affects the tooth-supporting tissues.
Poor oral hygiene: Infrequent brushing and inadequate interdental cleaning allow plaque to harden into tartar, promoting periodontitis.
Smoking: A major risk factor smoking reduces immune response and increases vulnerability to infection.
Genetic factors: Some people are genetically predisposed to periodontitis.
Chronic diseases: Poorly controlled diabetes increases susceptibility. Other conditions (such as heart disease and immune disorders) may also be associated with higher risk.
Medications: Some medications (like anticoagulants or those that reduce saliva) can increase risk.
Hormonal changes: Pregnancy, menopause, or hormonal contraception can increase gum vulnerability.
Stress: Stress can weaken immune defenses and increase susceptibility to gum infections.
Bleeding gums: natural approach for periodontitis
Treatment depends on severity. Options include:
Scaling and root planing: Professional deep cleaning to remove plaque and tartar; root planing cleans below the gumline to remove bacteria in periodontal pockets.
Antibiotics: May be prescribed to reduce infection and pain (local or oral).
Periodontal surgery: In advanced cases, surgery may be needed to repair gum and bone damage, including gum or bone grafts.
Rehabilitation and follow-up: Regular dental monitoring is essential to control the condition and improve gum health.
Bleeding gums: preventing periodontitis
Brushing + water flosser: Brush twice daily with a sonic toothbrush for improved effectiveness. Use an ozonated or fluoride toothpaste, and use an ozone water flosser daily to remove plaque and prevent tartar buildup.
Regular dental appointments: Routine check-ups and professional cleanings prevent plaque and tartar accumulation.
Quit smoking: Stopping tobacco use greatly improves gum health.
Balanced diet: Fruits and vegetables, fewer sugars supports teeth and gums.
Manage underlying conditions: Control diabetes and other conditions to reduce risk.
To conclude, periodontitis is a serious gum condition that can lead to tooth loss if left untreated.
It’s important to consult a dentist as soon as the first symptoms appear to avoid severe complications. Good oral hygiene and regular professional care can prevent and treat periodontitis effectively. The Aquolab product pack to fight periodontitis is your ally for daily oral hygiene.
🔹 Bleeding gums: brushing too hard
Brushing too vigorously can damage your teeth and gums, even if you’re trying to clean thoroughly. Here’s what can happen when you brush too hard:
Bleeding gums: brushing too hard
Gum recession: Aggressive brushing can push the gums back, exposing tooth roots. This can increase sensitivity to temperature changes and pain and may lead to more serious oral health problems.
Enamel wear: Enamel is the protective outer layer of the teeth. Brushing too hard with a stiff toothbrush can erode enamel, increasing the risk of cavities and sensitivity.
Tooth sensitivity: When enamel wears down and gums recede, more sensitive parts of the teeth become exposed, causing pain or discomfort especially with hot or cold foods and drinks.
Gum damage: Harsh brushing can cause cuts and irritation, making gums inflamed, red, and tender.
Periodontal pocket formation: Brushing too forcefully can contribute to pocket formation between teeth and gums, potentially worsening gum problems like gingivitis or periodontitis.
Bleeding gums: what to do
Use a soft-bristled toothbrush: Hard bristles are more abrasive. Soft bristles clean effectively without damaging gum tissues. Sonic toothbrushes have an ideal motion to protect the gums.
Don’t scrub hard: Vigorous scrubbing isn’t necessary. A gentle, oscillating motion top to bottom is recommended, especially along the gumline.
Use proper technique: Brush with gentle, oscillating movements, holding the brush at about a 45° angle to the gumline to remove plaque without irritating the gums. Avoid rotating brushes and prefer sonic brushes for a gentler routine.
Don’t force it: Brushing shouldn’t feel like physical effort. If you feel pain or bleeding, it may be a sign you’re brushing too hard.
Brush for 2 minutes: About 30 seconds per side, without force. A timer or an electric toothbrush with a built-in timer can help.
See a dentist: If you have gum problems or pain, consult a dentist to check for gum recession or technique-related damage.
To summarize, brushing should be gentle but effective. If you brush too hard, you risk damaging teeth and gums.
Using a soft-bristled toothbrush and adopting a gentle, correct technique are key to maintaining good oral hygiene without harming gum or tooth health. Sonic toothbrushes are ideal for daily hygiene.
🔹 Bleeding gums and medications
Some medications can increase the risk of gum bleeding by affecting oral health in different ways. Here are the main types of medications that may contribute:
Bleeding gums and anticoagulants
Anticoagulants such as warfarin (Coumadin), apixaban (Eliquis), rivaroxaban (Xarelto), or aspirin reduce normal blood clotting. This can increase bleeding risk, including in the gums. If you’re taking anticoagulants and have frequent gum bleeding, consult your dentist.What is the link between proton pump inhibitors (PPIs) and gum bleeding?
PPIs such as omeprazole (Prilosec) or esomeprazole (Nexium) treat acid-related conditions like reflux. These medications may interfere with blood clotting and increase the risk of gum bleeding, especially with long-term use.How do immunosuppressants affect the gums?
Medications used for autoimmune diseases or after organ transplants (such as cyclosporine, corticosteroids like prednisone, and other immunosuppressants) can cause swollen gums that bleed more easily.Why can antibiotics increase gum vulnerability?
Some antibiotics (like cephalosporins and amoxicillins) can disrupt the oral bacterial balance, increasing vulnerability to inflammation and infections, which can lead to gum bleeding.How do anti-epileptic drugs affect gums?
Medications such as phenytoin (Dilantin) or carbamazepine can cause gingival overgrowth, making gums more likely to bleed.Why can psychiatric medications interfere with gum health?
Some antipsychotics and antidepressants (for example fluoxetine or sertraline) may affect blood clotting or cause dry mouth, both of which can contribute to gum problems, including bleeding.Why can some blood pressure medications affect gum health?
Some antihypertensives especially ACE inhibitors like captopril or lisinopril can cause side effects such as mouth pain or gum bleeding, though this is less common.Why are alcohol-based mouthwashes irritating for gums?
Some mouthwashes containing alcohol can irritate gum tissues, making them more prone to bleeding. They can also dry out the mouth, which may promote bacterial growth and inflammation.
How to manage the risk of medication-related gum bleeding
Monitor bleeding: If you’re on medication and notice regular or heavy gum bleeding, tell your doctor or dentist. They can adjust treatment or recommend steps to reduce risk.
Maintain good oral hygiene: Brush gently with a soft-bristled toothbrush and use an ozone water flosser daily to remove plaque and prevent bacterial buildup that can worsen gum inflammation.
Regular dental check-ups: If you take medications that affect gums, regular oral exams help detect issues early and prevent complications.
Mouthwash and hydration: Use alcohol-free mouth rinses and drink enough water to reduce dryness and bleeding risk.
To summarize, if you’re taking medication and notice gum bleeding, it’s important to consult your doctor or dentist.
They can adjust your treatment and advise the best practices to protect your gums.
🔹 Bleeding gums and nutritional deficiencies
Nutritional deficiencies can significantly affect gum health and lead to bleeding. Certain vitamins and minerals are essential for maintaining oral health, and when they’re lacking, gums can become weaker and more prone to inflammation and bleeding.
Bleeding gums and nutritional deficiencies
Bleeding gums and vitamin C deficiency (scurvy)
Vitamin C is essential for gum health. It supports collagen production, which helps maintain connective tissues, including gums. A deficiency can cause severe gingivitis, swollen red bleeding gums, and in serious cases even tooth loss.
Symptoms of vitamin C deficiency:
Swollen, red, bleeding gums, especially during brushing or flossing.
Gum pain and tenderness.
Formation of gum pockets.
Loose teeth.
Fatigue, general weakness, dry skin.
Vitamin C–rich foods:
Citrus fruits (oranges, grapefruit, lemons).
Kiwi, strawberries, mango.
Vegetables like bell peppers, broccoli, Brussels sprouts, spinach.
Bleeding gums and vitamin D deficiency
Vitamin D is crucial for bone health, including the jawbone that supports teeth. Deficiency can weaken bones and increase the risk of periodontal disease and tooth loss.
Symptoms of vitamin D deficiency:
Muscle and bone pain.
More sensitive teeth and gums.
Higher risk of cavities and gum disease.
Vitamin D–rich foods:
Fatty fish (salmon, mackerel, sardines).
Egg yolks.
Fortified milk and fortified orange juice.
Sun-exposed mushrooms.
Bleeding gums and vitamin K deficiency
Vitamin K plays a key role in blood clotting. A deficiency can increase gum bleeding risk. It also supports bone and soft tissue health, including gums.
Symptoms of vitamin K deficiency:
Excessive gum bleeding.
Easy bruising.
Frequent nosebleeds.
Vitamin K–rich foods:
Leafy greens (kale, spinach, broccoli).
Cabbage, lettuce, and other cruciferous vegetables.
Soybean oil and canola oil.
Bleeding gums and calcium deficiency
Calcium is essential for teeth and bones. A deficiency can weaken teeth and gums, contributing to gum recession and tooth mobility.
Symptoms of calcium deficiency:
Fragile teeth, increased cavities.
Sensitive gums that bleed easily.
Higher risk of gum disease.
Calcium-rich foods:
Dairy products (milk, cheese, yogurt).
Leafy greens (kale, broccoli).
Tofu, chia seeds, almonds.
Bleeding gums and folate deficiency (vitamin B9)
Folate supports cell regeneration, including gum tissue cells. A deficiency can cause inflamed, bleeding gums and increase periodontal risk.
Symptoms of folate deficiency:
Red, swollen gums that bleed easily.
Gum tenderness and pain.
Fatigue and weakness.
Folate-rich foods:
Leafy greens (spinach, lettuce, broccoli).
Beans, peas, lentils.
Citrus fruits, avocado, beets.
Other minerals important for gum health
Zinc: Supports tissue repair and immune defense. Deficiency can increase gum infection and bleeding risk.
Iron: Important for red blood cells and tissue health. Deficiency can contribute to gingivitis and increased gum sensitivity.
Bleeding gums: preventing dietary deficiencies
Balanced diet: Eat a variety of foods rich in essential vitamins and minerals for oral health.
Supplements: If you struggle to meet needs through food, a doctor or nutritionist can recommend supplements.
Dental follow-up: Regular check-ups help detect gum issues early and treat them before they worsen.
Avoid tobacco: Smoking can worsen gum issues by reducing absorption of nutrients and decreasing gum blood flow.
To summarize, nutritional deficiencies especially in vitamins C, D, K, calcium, folate, and zinc can cause gum bleeding, inflammation, and infections.
Maintaining a diet rich in these nutrients helps prevent problems and supports good oral health. If you have concerns, consulting a healthcare professional is essential for proper diagnosis and treatment. Keep a good oral hygiene routine: brush with a soft-bristled sonic toothbrush and use an ozone water flosser daily to remove plaque and prevent bacterial buildup that can cause gum inflammation.
🔹 Bleeding gums and hormonal changes
Hormonal changes can significantly impact gum health, leading to bleeding and other oral issues. These changes can occur during puberty, pregnancy, menopause, or while using hormonal treatments.
Here’s an overview of the main phases when hormones can affect gums and cause bleeding:
Bleeding gums and puberty
During puberty, hormone levels especially estrogen and progesterone rise significantly, making gums more sensitive and prone to inflammation.
Effects: Gums may become red, swollen, tender, and bleed more easily, especially when brushing or flossing.
Aggravating factors: Teenagers may pay less attention to oral hygiene, worsening gingivitis symptoms.
Bleeding gums and pregnancy
Pregnancy causes major hormonal fluctuations, particularly in estrogen and progesterone, affecting how gums respond to plaque.
Effects: Pregnancy gingivitis may occur, with swollen, red, tender gums that bleed easily.
Aggravating factors: Nausea/vomiting and dietary changes can make oral hygiene harder, increasing inflammation risk.
Prevention: Maintain good oral hygiene and see a dentist regularly during pregnancy.
Bleeding gums and menopause
Menopause reduces estrogen and progesterone production, impacting gum and bone health.
Effects: Lower hormone levels can increase vulnerability to inflammation and infection, leading to gum bleeding. Some may develop atrophic gingivitis, making gums more fragile and sensitive.
Associated symptoms: Dry mouth can worsen gum problems and increase infection and bleeding risk.
Prevention: Maintain good oral hygiene, use appropriate toothpaste, see a dentist regularly, and drink enough water to limit dryness.
Bleeding gums and hormonal contraceptives (pills, implants)
Hormonal contraceptives can cause hormonal fluctuations similar to pregnancy/puberty, making gums more sensitive to infection.
Effects: Increased risk of gingivitis and gum bleeding.
Aggravating factors: Some may accumulate plaque more easily due to biological changes.
Bleeding gums and premenstrual syndrome (PMS)
Hormone shifts (especially progesterone) can increase gum inflammation and bleeding tendency.
Effects: Some experience gingivitis-like symptoms or sensitive, bleeding gums during the premenstrual phase.
How do hormonal changes cause gum bleeding?
Inflammatory response: Estrogen and progesterone influence how gums react to bacterial plaque, increasing inflammation.
Blood flow: Hormones increase gum blood flow, making gums more swollen and prone to bleeding.
Immune response: Hormones can alter immune response, increasing susceptibility to gingivitis and periodontitis.
How to prevent gum bleeding linked to hormonal changes
Good oral hygiene: Brush twice daily with a soft-bristled sonic toothbrush and use an ozone water flosser to prevent plaque buildup.
Regular dental visits: Especially during puberty, pregnancy, or menopause, to monitor gum health.
Hydration: Drink enough water to reduce dry mouth and bad breath risk.
Avoid tobacco: Smoking worsens hormonal effects on gum health.
Balanced diet: Prioritize vitamins and minerals for gum health, especially vitamin C and calcium.
To summarize, hormonal changes can make gums more vulnerable to inflammation and bleeding especially during puberty, pregnancy, menopause, or hormonal contraception use.
Good oral hygiene and regular dental care are essential to prevent gum problems from worsening.
🔹 Bleeding gums and tobacco
Smoking is a major factor that harms oral health and can cause serious issues, including bleeding gums. Tobacco use affects gums, slows healing, and can worsen periodontal disease.
Bleeding gums caused by tobacco
Reduced blood flow to gums: Smoking decreases blood circulation in gum tissues, reducing oxygen and nutrient supply.
Effect: Gums become more fragile and prone to bleeding when irritated.Weakened immune system: Smoking reduces the body’s ability to fight infections, including gum infections.
Effect: Higher risk of gingivitis and periodontitis, often with swollen bleeding gums.More plaque and tartar buildup: Tobacco promotes plaque and tartar accumulation and irritates gum tissue.
Effect: Increased inflammation and bleeding.Reduced healing capacity: Smoking slows gum healing after irritation or dental treatment (like scaling).
Effect: Longer-lasting bleeding and delayed recovery.Higher risk of periodontitis: Smokers are more likely to develop advanced gum disease.
Effect: Easy bleeding, gum pain, loose teeth, persistent bad breath.Reduced perception of symptoms: Tobacco can dull gum sensitivity, so symptoms go unnoticed longer.
Effect: Delayed dental consultation until the condition becomes severe.
Impacts of tobacco on oral health
More gum infections.
Bad breath (halitosis).
Tooth loss (if periodontitis progresses).
Higher risk of oral cancer.
How to reduce tobacco’s impact on gums
Quit smoking: The best step to improve gum health.
Strict oral hygiene: Brush twice daily with a sonic toothbrush; use an ozone water flosser daily; consider an antiseptic toothpaste such as OZONIC (ozone-based).
Regular dental visits: Professional cleanings remove tartar that brushing can’t.
Antibacterial mouthwash: Prefer alcohol-free options, as alcohol-based mouthwashes can be harsh.
Balanced diet: Vitamins and minerals (especially vitamin C and calcium) support gum repair.
To summarize, smoking greatly increases the risk of gum bleeding and periodontal disease.
It reduces blood flow, weakens immunity, and makes gums more vulnerable to infections. Protect your gums by quitting smoking, maintaining strong oral hygiene, and seeing a dentist regularly.
🔹 Bleeding gums and diabetes
Diabetes can strongly impact oral health and is closely linked to gum bleeding. People with diabetes especially when blood sugar is poorly controlled are more vulnerable to infections, including gum disease, which can cause bleeding.
Here’s how diabetes can affect gums and lead to bleeding:
Bleeding gums: diabetes increases gum disease risk
Poorly controlled diabetes increases the risk of gingivitis and periodontitis. It weakens immune defenses, making gum infections harder to fight.
Effect: More gum inflammation and frequent bleeding, especially with brushing or flossing.Why does diabetes reduce gum healing?
High blood sugar can slow tissue repair, including in the gums.
Effect: Fragile gums, slower healing after irritation or dental care, and persistent bleeding.Why does diabetes increase plaque and tartar?
People with diabetes may have thicker saliva, which can promote plaque and tartar buildup.
Effect: More irritation, swelling, and bleeding; plaque can harden into tartar if not removed.Why does diabetes increase inflammation and gum bleeding?
Uncontrolled diabetes can intensify gingival inflammation, an early stage of gum disease.
Effect: Swollen irritated gums bleed more easily; untreated gingivitis can progress to periodontitis.What is the two-way relationship between diabetes and gum disease?
Gum disease can worsen blood sugar control, and poor blood sugar control can worsen gum disease.
Effect: Periodontal inflammation can increase stress hormones and insulin resistance, making glucose harder to manage.
Bleeding gums: preventing issues related to diabetes
Control blood sugar: Stable, well-controlled glucose reduces oral complications.
Strict oral hygiene: Brush twice daily with a sonic toothbrush, use ozonated or fluoride toothpaste, and add an ozone water flosser daily. Brush gently to avoid irritation.
Antiseptic mouthwash: Can help reduce plaque and infections.
Regular dental visits: Routine exams and cleanings prevent tartar buildup and detect gum issues early.
Quit smoking: Smoking is a major risk factor, especially in diabetes.
Balanced diet: Vitamins and minerals (especially vitamin C and calcium) help gum resistance and healing.
Stress management: Stress can worsen blood sugar control and gum health.
In summary, poorly controlled diabetes is a major factor for gum problems, including bleeding.
Because of reduced circulation, altered immunity, and plaque buildup, people with diabetes are more likely to develop gum infections. Prevention relies on good glucose control, strong daily oral hygiene, regular dental care, and a healthy lifestyle.
Continue reading...
© 2024. All rights reserved.