hygiene-precision: distributor of Aquolab products
Peri-implantitis: Symptoms and Treatments of the Infection
Pain, bleeding or swelling around your dental implant? Discover the symptoms of peri-implantitis and how to treat this infection.
hygiene-precision.com
5/6/20265 min read
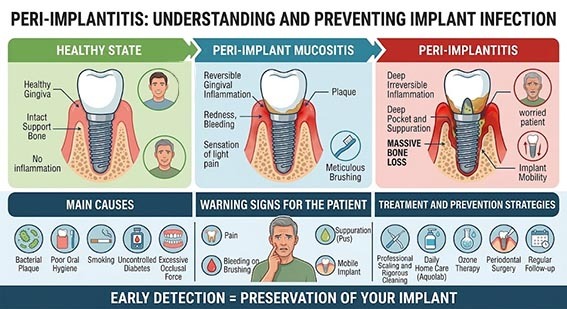
Peri-implantitis: everything you need to know about dental implant infection
Are you experiencing unusual pain , swelling, or bleeding gums around your prosthesis? Be aware that these could be the first signs of a dental implant infection . While implants are an aesthetic and long-lasting solution, they are unfortunately not immune to bacterial attacks.
If the inflammation remains superficial, it is called peri-implant mucositis , a condition that is fortunately reversible. However, without prompt treatment, it can develop into peri-implantitis . This much more serious condition directly attacks the bone tissue supporting the implant, significantly increasing the risk of loosening and loss of the prosthesis.
Don't let worry take hold. Discover how to identify the symptoms of this disease, its causes, and most importantly, what treatment for peri-implantitis to adopt to protect your implants in the long term.
This article contains the following:
Pain after a dental implant: normal or worrying?
Pain following a dental implant procedure is common. It is related to tissue healing and the body's normal reaction.
How long does the pain last?
3 to 5 days on average
Gradual decrease after 48 hours
Sensitivity may last up to 1 to 2 weeks
⚠️ On the other hand, persistent or intensifying pain may signal a dental implant infection or the beginning of peri-implantitis .
Peri-implantitis: definition and difference from peri-implant mucositis
Peri -implantitis is an inflammation of the tissues around the implant, affecting both the gum and the bone, with possible formation of a periodontal pocket .
Not to be confused with peri-implant mucositis :
Mucositis : superficial, reversible inflammation without bone involvement
Peri-implantitis : deep inflammation with irreversible bone loss
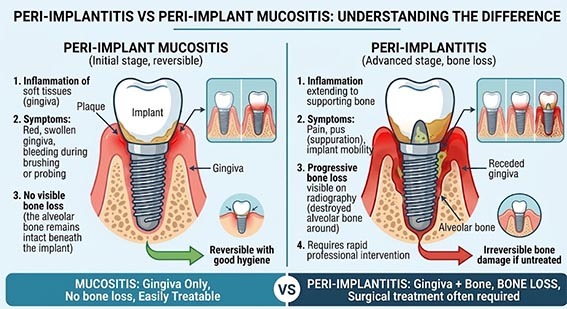
Symptoms: How to recognize peri-implantitis
The signs may be subtle at first, but certain symptoms should raise concern:
Bleeding gum around the implant
Redness and swelling (inflammation)
Persistent dental implant pain
Bad breath linked to bacterial plaque
Presence of pus
Sensation of looseness or dislodgement of the implant
👉 The presence of tartar and biofilm promotes the worsening of these symptoms.
What are the causes of peri-implantitis?
1. Insufficient oral hygiene
The accumulation of bacterial plaque around the implant is the main cause. Without proper brushing and effective interdental cleaning, bacteria cause chronic periodontal inflammation.
2. General risk factors
Tobacco (reduced blood flow)
Poorly controlled diabetes
Inflammatory diseases
3. Mechanical factors
Poor distribution of forces
Excess cement
Implant incorrectly positioned
Diagnosis of peri-implantitis
The diagnosis is based on:
Clinical examination (bleeding, inflammation)
Measurement of periodontal pockets
X-ray to assess bone tissue loss
Regular monitoring allows for the detection of peri-implant mucositis before it develops into peri-implantitis.
Treatments: How to treat an infection under an implant
The treatment of peri-implantitis depends on the stage:
Non-surgical phase
Plaque and tartar removal
Disinfection (ultrasound, laser, sometimes ozone)
Improved oral hygiene
Surgical phase
Deep cleaning
Pocket reduction
Bone tissue regeneration (grafting)
🎯 Objective: to stop the infection and prevent the implant from becoming dislodged
Prevention: Hygiene routines to protect your implants
The French Union for Oral Health (UFSBD) recommends using a water flosser as a useful complement to removing plaque between teeth and under the gum line , where a regular toothbrush is insufficient for daily use. The water flosser, with its controlled pressure, is gentler and kinder to the gums than interdental brushes .
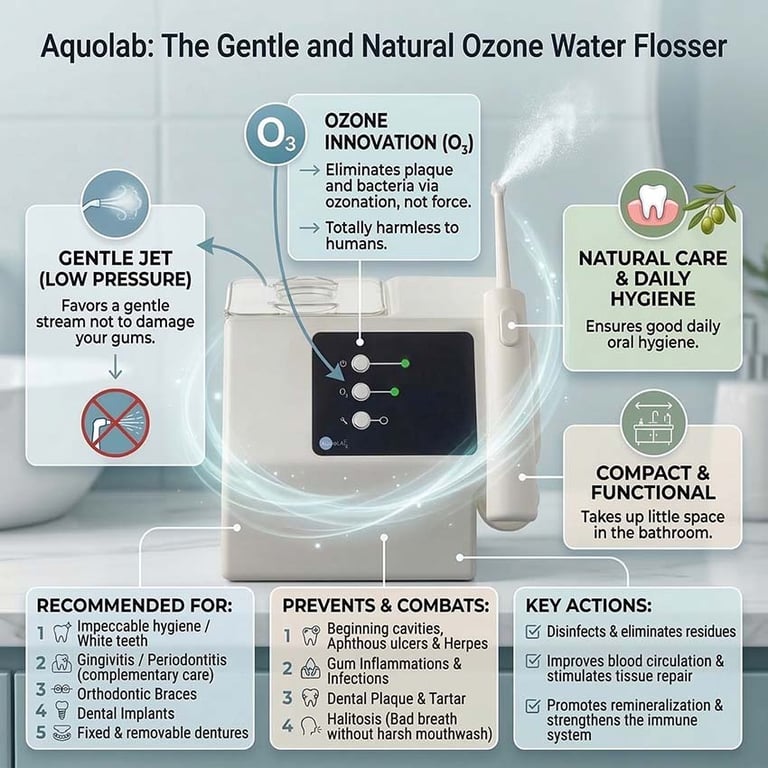
The ozone dental irrigator: your best ally
The Aquolab ozone dental jet
stands out as an innovative solution
for deep cleaning around dental implants .
Thanks to the micro-diffusion of ozonated water , it allows for gentle and natural disinfection
of interdental spaces, gums, and peri-implant areas.
Why ozone?
Ozone has effective antibacterial and disinfectant properties against dental plaque , significantly reducing bacteria responsible for cavities, gingivitis and oral infections, while complementing conventional brushing ( study on ozonated water and dental plaque ; review on ozone in dentistry ).
When used in oral hygiene, ozone contributes to:
to eliminate the anaerobic bacteria responsible for peri-implantitis without damaging the titanium of the implant
Limit gum inflammation
Improve the feeling of cleanliness and freshness
The Aquolab ozone dental jet can therefore be perfectly integrated into the daily routine of patients with dental implants , in addition to brushing and professional check-ups.
A four-year study demonstrates that thanks to Aquolab ozonated water, used before and for three weeks after dental implant placement, the mouth benefits from deep , natural, and safe disinfection. This technology creates ideal conditions for healthy healing and a stable result, for a long-lasting implant . Source: 2018_08_21_Marconcini_et_al-2018-Clinical_Implant_Dentistry_and_Related_Research
The importance of thorough brushing
Aquolab products for optimal implant hygiene
Aquolab offers a range of complementary products designed to optimize the oral care of dental implants.
Ozonic ozone toothpaste
Aquolab's Ozonic toothpaste contains stabilized ozone microbubbles
and gum-friendly ingredients. Daily use helps to:
Maintaining a healthy oral environment
Reduce the formation of bacterial plaque
Protecting sensitive peri-implant tissues
Promote remineralization
It is perfectly suited to patients prone to mucositis or peri-implantitis , who are looking for a non-abrasive and soothing toothpaste.
The UFSBD recommends the use of an electric toothbrush to improve brushing efficiency while respecting sensitive gums.
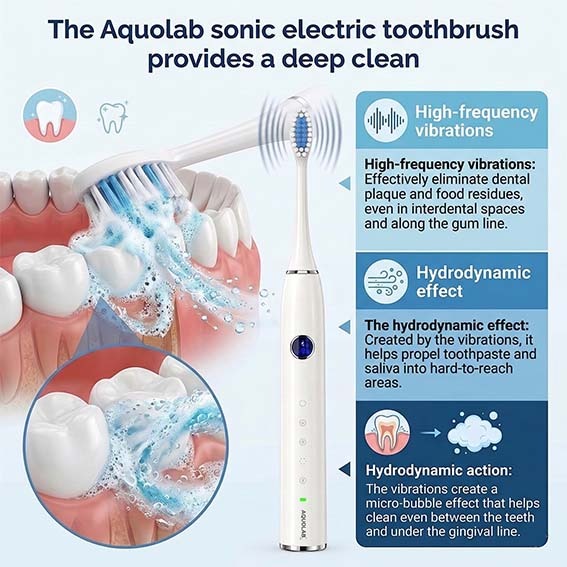
The Aquolab sonic toothbrush
The Aquolab sonic toothbrush offers high-frequency brushing
to effectively remove plaque, even in hard-to-reach areas around implants. Thanks to its gentle and precise movements , it promotes impeccable hygiene without traumatizing gums, which are often more fragile around implants.
Prevention: the key to preventing peri-implantitis
Good prevention relies on a rigorous implant hygiene routine :
Essential actions
Brush 2 to 3 times a day
Use interdental brushes if you don't have a water flosser. Be careful with your gums!
Cleaning with a water flosser
These actions help to eliminate bacterial plaque before it turns into tartar.
When to consult a doctor?
Check quickly if you observe:
Persistent inflammation
Bleeding gum around the implant
An unusual pain
A feeling of mobility
Early diagnosis often allows treatment of peri-implantitis without major surgery.
Conclusion: Preventing peri-implantitis on a daily basis
Peri -implantitis is not inevitable. It is directly linked to the balance between bacteria, hygiene and periodontal health .
Adopting a complete routine including brushing , water flosser , and possibly the use of ozone -based solutions , helps to limit the risks of dental implant infection and prevent implant loosening .
👉 Rigorous daily maintenance is the best guarantee for keeping implants healthy and long-lasting.
Continue reading...
© 2024. All rights reserved.