hygiene-precision: distributor of Aquolab products
Stomatitis: Causes, Symptoms and Treatments
What is oral stomatitis? Discover its causes, symptoms, and our natural solutions (ozone therapy) to quickly relieve the pain.
hygiene-precision.com
5/6/20265 min read
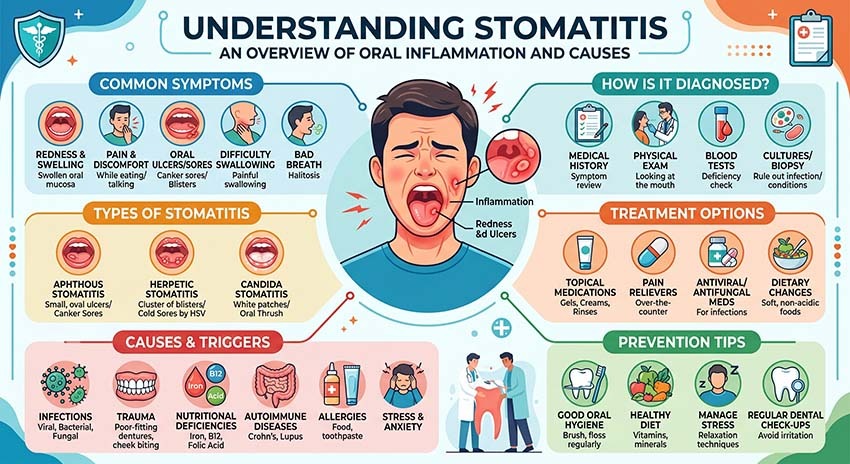
Stomatitis: definition, causes and treatments
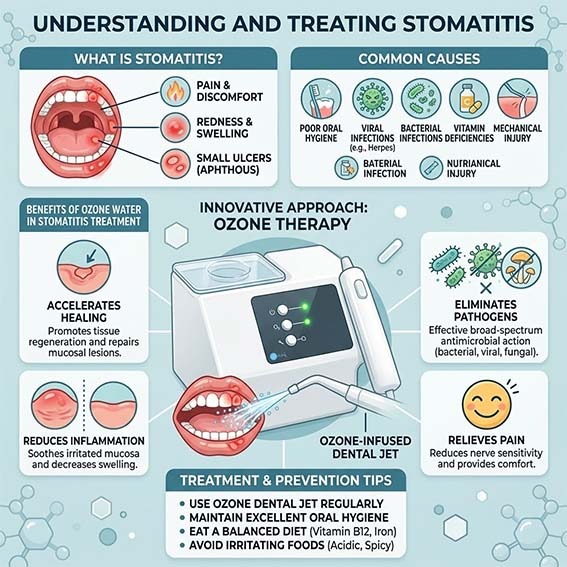
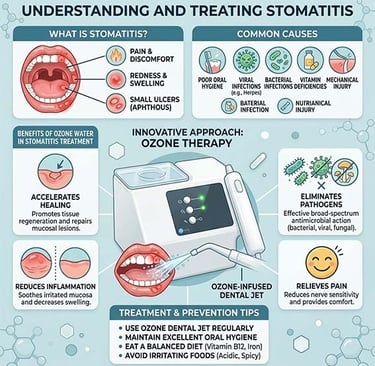
Stomatitis is an inflammation of the oral mucosa , the tissue lining the inside of the mouth. It can be painful and appear in various areas: the palate, tongue, inside of the cheeks , and base of the gums. Understanding its causes, symptoms, and effective ways to relieve it is essential for regaining optimal oral comfort.
This article contains the following:
Stomatitis definition
Stomatitis encompasses various forms of inflammation affecting the mouth . It often manifests as sores, redness, or ulcerations , causing significant discomfort when chewing, speaking, or even at rest . This condition can be occasional or recurrent , depending on its cause.
Stomatitis symptoms
Oral pain : ranging from mild discomfort to intense pain.
Redness and inflammation : the affected area appears irritated.
Wounds and ulcers : similar to canker sores, sometimes more extensive.
Swelling : swollen areas that are tender to the touch.
Difficulty eating or swallowing : due to inflammation.
Other signs : fever, fatigue, altered sense of taste or smell.
What are the different types of stomatitis?
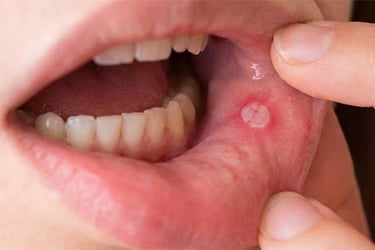
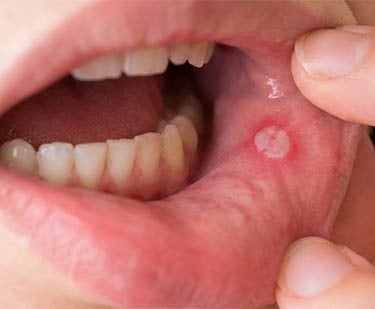
Aphthous stomatitis
The most common type involves small, painful lesions ( canker sores ).
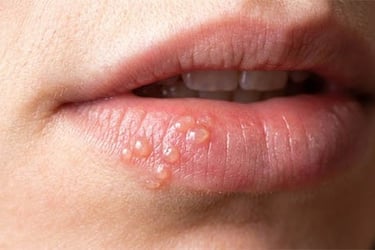
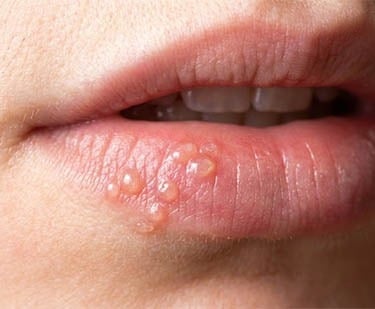
Herpetic stomatitis
Caused by the herpes virus, accompanied by blisters that can ulcerate.
Candidal Stomatitis (Thrush)
Candidal stomatitis, more commonly known as thrush, is characterized by white patches on the tongue and inside of the mouth, caused by a fungal infection.
Prosthetic stomatitis
Related to poor hygiene or improper fitting of dentures.
Angular stomatitis
Cracks and redness at the corners of the lips, often seen in children and the elderly.
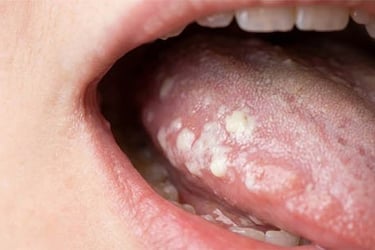
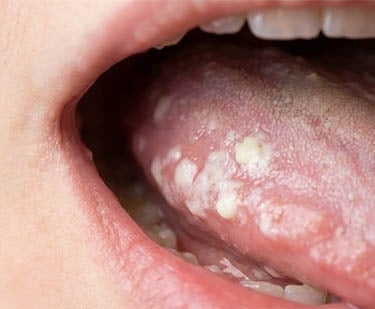
Stomatitis causes
Viral infections : herpes simplex virus (HSV), Coxsackie virus.
Bacterial infections : streptococci, staphylococci.
Fungal infections : oral candidiasis (thrush).
Trauma : bites, burns, accidental injuries.
Allergies : to certain foods or medications.
Nutritional deficiencies : deficiency in vitamin B12, iron, folic acid.
Side effects of treatments : chemotherapy, radiotherapy, certain medications.
Stomatitis treatment: How to relieve and treat a mouth sore related to stomatitis?
Treatment depends on the cause, but several solutions can reduce inflammation and accelerate healing:
Antiviral, antifungal or antibiotic medications depending on the origin of the infection.
Pain relievers or local anesthetic gels to calm the pain.
Antiseptic mouthwashes to reduce bacteria and promote healing.
Using an ozone water flosser , such as the Aquolab , to naturally deep clean , disinfect the oral cavity and quickly relieve sores .
Hydration and a gentle diet to avoid worsening the damage.
Natural treatment for stomatitis: Ozone to treat bleeding in the mouth and accelerate healing
Oral ozone therapy is increasingly used in dental hygiene. Thanks to its antibacterial, antiviral, and anti-inflammatory properties, ozone helps to:
Eliminate the pathogens responsible for stomatitis.
Reduce bleeding in the mouth , especially in the gums.
Accelerate the healing of mouth wounds and ulcers.
Relieve pain and inflammation from the first use.
Treat stomatitis and oral infections with the Aquolab ozone water jet
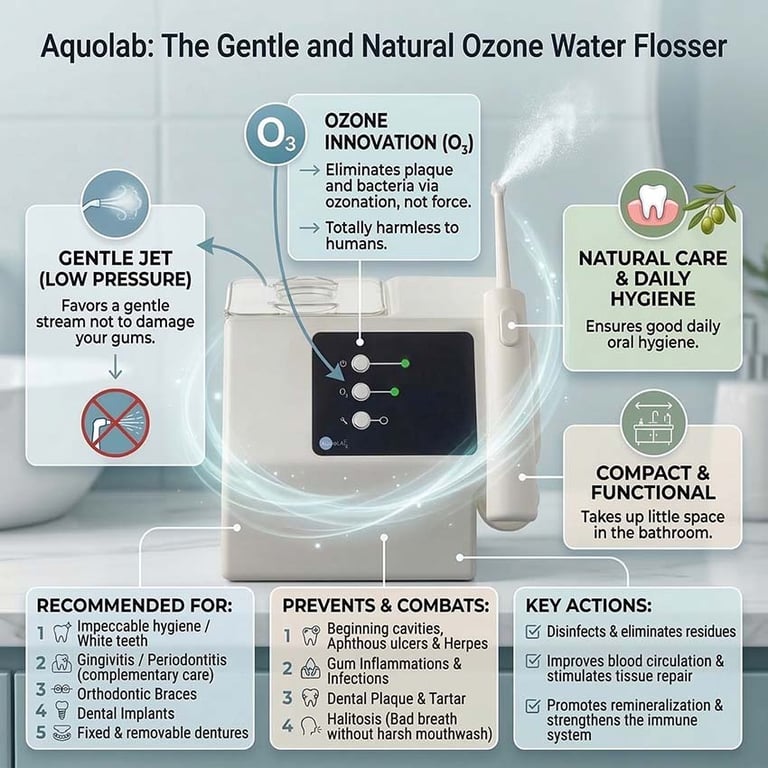
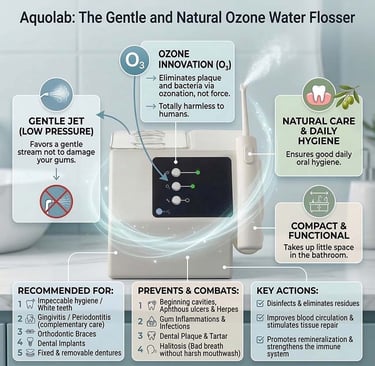
When faced with stomatitis or an oral infection, daily hygiene often becomes painful. This is where the Aquolab ozone water flosser offers a revolutionary and natural solution . Unlike traditional water flossers that use strong mechanical pressure, potentially damaging already fragile mucous membranes, the Aquolab uses a very gentle jet of water to avoid harming your gums .
Its real advantage lies in the addition of ozone , a powerful natural disinfectant harmless to humans. Ozone-enriched water acts directly on lesions and ulcerations, effectively eliminating dental plaque and infection-causing bacteria, all at low pressure .
Beyond simple chemical-free cleaning, ozone therapy offers genuine therapeutic benefits . It improves local blood circulation and stimulates the repair of damaged tissues, significantly accelerating the healing of stomatitis. Finally, its action strengthens the oral immune system and promotes remineralization. Equipped with a specific nozzle for sensitive mouths (0.8 mm), this durable and eco-friendly water flosser provides daily relief from inflammation and effectively prevents recurrence .
Testimonials from a user:
"I bought the Aquolab ozone water flosser six months ago. The results are fantastic: no infections, cavities, etc. I've eliminated all the problems I had before using Aquolab." RM
Example of an infection case treated with the Aquolab ozone dental jet:
Aquolab has demonstrated the effectiveness of its ozone dental jet in treating oral infections such as black hairy tongue. Sources: 2017_08_Aquolab - case report_lingua nigra_Dott.ssa Casu_Cagliari_NN STAMPARE_ INGLESE
Here are the key points to remember:
Effectiveness and speed : A single session resulted in almost total remission in just one week.
Antimicrobial action : Ozonated water has proven more effective than conventional treatments, such as clotrimazole, in reducing the presence of microbes.
Safety and comfort : This treatment has no side effects. It is less toxic to tissues than standard products and provides immediate relief from burning sensations.
Stomatitis: Treating and Preventing It: 5 Essential Natural Hygiene Tips
Maintain excellent oral hygiene : gentle and sonic brushing preferably 2 to 3 times a day, regularly use an ozone toothpaste for perfect oral disinfection.
Use an ozone dental jet to disinfect your mouth, treat sores and remove plaque from between teeth.
Avoid irritants : spicy foods, acidic drinks, tobacco and alcohol.
Adopt a balanced and gentle diet : rich in vitamins and minerals, avoid hard and aggressive foods.
Drink enough water to maintain good hydration of the oral mucosa.
Conclusion
Stomatitis can quickly become bothersome and painful, but there are effective solutions to relieve it and promote rapid healing. In addition to appropriate medical treatments, ozone is a powerful, natural solution for disinfecting, soothing pain, and treating sores and bleeding in the mouth .
Maintaining optimal oral hygiene remains the best prevention against recurrent stomatitis.
Continue reading...
© 2024. All rights reserved.